
CATEGORIES:
BiologyChemistryConstructionCultureEcologyEconomyElectronicsFinanceGeographyHistoryInformaticsLawMathematicsMechanicsMedicineOtherPedagogyPhilosophyPhysicsPolicyPsychologySociologySportTourism
Functional symptomes
1. Change of mobility and form of the shadows as a result breathing.
2. Mobility of the diaphragm cupulas, paradoxical motion of diaphragm.
3. Change of radiolucency of pulmonary tissue at deep inhalation and exhalation(see fig 15.11)
4. Signs of bronchial obstruction. There are three degrees of bronchial obstruction: partial obstruction, valval obstruction and complite obstruction.
a) partial obstruction - roentgenological hypoventilation (1 degree of bronchial obstruction);
b) valval obstruction - roentgenological emphysema (2 degree of bronchial obstruction);
c) complete obstruction - roentgenological – atelectasis (3 degree of bronchial obstruction).
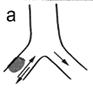
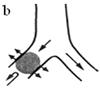
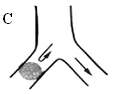
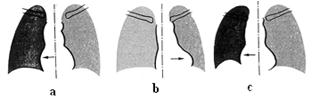
Fig.15.11 Degrees of violation of the bronchial communicating.
а) partial (hypoventilation); b) valvular (emphysema); c) complete (atelactics)
Correct interpretation of the got x-ray information, in combination with a clinic instrumental help to establish the exact diagnosis. Only deep understanding of roentgenological pattern - objective reflection of the pathomorphological substrates allows to carry out sindromic, between syndromic and intrasyndromic diagnostics in a number of organs diseases and system diseases of an organism.
Syndromes of pulmonary pathology
1. Extensive shadow of pulmonary tissue (see fig 15.12) is shadow, which occupies more than a 2/3 pulmonary field, there are a loss of airness of whole lung or lobe, at the accumulation of liquid in a pleura cavity.
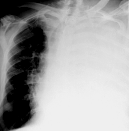
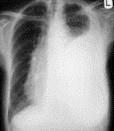
Fig.15.12. Total and subtotal shadows
Differences between intrapulmonary process from extrapulmonary.
Intrapulmonary processes
Inflammatory process is lobar if a form of shadow is in character of lobe with air bronchogram effect, heterogeneous shadow has clear-defined border due to interlobar pleura and volume of lung is not diminished.
Atelectasis of lobe is suspected if homohenous shadow has form of lobe and has clear-defined border (due to interlobar pleura) and volume of lung decreases.
Extensive pleuritis is suspected if a form of homohenous shadow is’t in character of any lung’s part, maximal intensivity of shadow locates in the inferior part of hemithorax and form of shadow differs according to the position in space, the organs of mediastinum displaces in a healthy side.
2. Local shadow of pulmonary tissue is shadow which occupies part of lung by volume between 1/3 and 2/3 lung’s volume (see fig 15.13) - lobe or segment or subsegment. The anterior and lateral projections are used for determining a form and a localization shadow. If it correspond to localization of lobe or segment - it is an intrapulmonar process; in difficult cases it is necessary to use polyposition and polyprojection examination of patient.
Encapsulated liquid in interlobar fissura in lateral projections has a form of biconvex lens, form of triangle (in the projection of interlobar fissura).
Local shadow may to locale near thoracic wall and near mediastinum. In these cases need to differentiate between extrapulmonary and intrapulmonary injuries: if conceptional center of shadow locates in lung that is the intrapulmonary injuries.
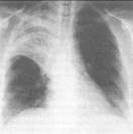

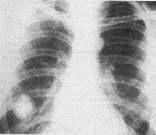
Fig.15.13. the limited reduction and spherical shade
3. Spherical shadow of pulmonary tissue
The spherical shadow is shadow of lung more than 1 cm in a diameter. It necessary describes according to PO-NU-FO-SI IN-PA-KO-S too. If a form is rounded, correct, contours are clear, a structure is homogeneous, that maybe bening tumour or cyst; if a form is wrong, contours are unclear – it maybe a malignant tumour; if a cavity with a horizontal level are present within the shadow - it is an abscess; if calcification is within the shadow and foci is around shadow that is tuberculoma. If a shadow is situated near the thoracic wall and it conceptional center is outside of thorax - it is an encapsulated costal pleurisy or pleural mesothelioma, If a shadow is situated near the thoracic wall and it conceptional center is outside of thorax; if a shadow adjoins to mediastinum, does’t separate from him and it conceptional center is in mediastinum – it is the mediastinal pathology.
4. Linear shadow of pulmonary tissue
The linear shadows of interlobar pleura (see fig 15.14) - linear shadows are the result of fibrosis as a consequence inflammatory processes (a contour will be unclear). Linear shadows may to have interlobar localization. Linear shadows may to arise up as a result of vessels’ and bronches’ pathologies – a lung’s stasis, a chronic bronchitis). Linear shadows maybe to running from tumour to the periphery together with bronches or lymphatic vessels around their.
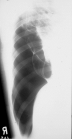
Fig.15.14. Linear shades
5. Focal, limited and widespread dissemination.
Foci are the small radioopaque area less then 1 cm. Their forms are various: maybe spheric or irregular shape ( see fig 15.15). Take into account prevalence of focus, their contours and intensity, condition of lung pattern around foci. If foci are localized in the area of apex and above a clavicle - it is more frequent to be tubercular; in inferior segments - more characteristically for pneumonia. If contours of foci are unclear this more typically for the nonspecific inflammation; if contours of foci are learer this more typically for the tuberculosis. Widespread in the eigther lungs, sizes 1-2 mm, round foci on apexes of lungs are typically for the acute tubercular dissemination. Various sizes of foci, more frequent rounded, clear, dense are met on both sides or are often spreaded near the diaphragm – are typically for metastatic injuries.
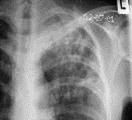
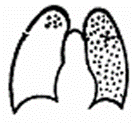
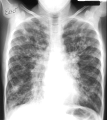
Fig.15.15. Focal and disseminated shades
It is important to estimate intensity of foci, a small and middle closeness is more frequent at pneumonia and tuberculosis. Lokalisation of pathological process and loud speaker of pathological changes have the defined value. Pneumonia resolves quickly, and tubercular changes are saved for months. If in a focus there are calcareous depositions it is the sign of old tuberculosis.
A small rounded shade can be the sign of lungs cancer, for determination of the shades structure it is necessary to do tomography. The sizes of tumour are increased in course of time. At pneumonia and tuberculosis foci are plural, and at a primary lungs tumour are single.
Widespread foci can be becous of at the professional diseases of the lungs - but they are more frequent in the middle departments of the lungs, on a background pneumosclerosis, in anamnesis - a work in dustinal conditions. Foci more frequent the shallow, nodeted shades, which well appeared on the sciagrams of the body, executed by a short exposition.
7. Pathology of the lung pattern
Anatomic substrates of the lung pattern are the blood vessels, bronches, lymphatic vessels, peribronchial and perivascular conecting tissue, and lymphatic nodes. In norm the lung pattern image is predefined mainly by blood vessels. At the pathology of each enumerated elements lung pattern changes (see fig 15.16 a, b).
Distinguish limited, widespread and total lung pattern change. He can increase - if vessels are spread (stagnation) or enriched (if the amount of vessels are increased in unit of area or volume lungs due to the increase of shallow vessels).
The lung pattern can be impoverished at emphysema lungs. A lung pattern can relax, if it recoveres shallow foci.
A lung pattern can be deformed in combination of strengthening with incorrect motion of vessels through scar development of the connecting tissue in intermediate stroma. There can be Kerli lines of at mitral stenosis - in inferior departments, lateral horizontal strips long to 2-2,5 and breadthways 1-2mm due to an interstitial edema.
a 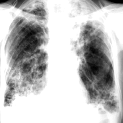 b
b  c
c 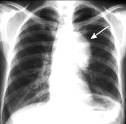
Fig.15.16. Pathological changes of lung pattern (a,b)and lungs root (c)
8. Pathological changes of the lungs roots
Shades of root lungs are mainly predefined by pulmonary artery on a sciagram; however root lungs consist of large bronches, lymphatic nodes, and cellulose. Each of these elements can change and a root can change as a result of it. Changes of root lungs can be independent or accompany to other diseases (see fig 15.16 c).
A width of the right root is 1-1,5 sm, length 6-8 sm, to the left part of it is a heart recovered. Between the right root and shades of the heart there is a light strip - a Prozorov path - a road clearance to the inferior lobular bronchus.
Necessarily take into account prevalence of changes - one- or bilateral defeat of root, is combined with other processes in lungs, eyelids of patient; contours and structure of root. Children more frequent have a one-sided defeat at tuberculosis, for adults more frequent at cancer. Polycyclic contours specify on the defeats of lymphatic nodes, unclear on infiltration of cellulose at inflammation or germination of tumour. Combination of root expansion with atelectasis can be at tumular bronchoadenitis and tumour.We can observed calcification of the lymphatic nodes.
9. Syndrome of the limited ring shades or cavities (see fig. 15.17.). Anatomic cavities in lungs are characterised by ring shades with air inwardly (Fig.15.17.). It is important to set their topography, because cavities can simulate changes in ribs and joints in a pleura cavity. In lungs a cavity can have thin even walls without a liquid, which is typical for an air cyst, if around are foci and strengthening lung pattern or fibrous lineas - it is a cavity.During an abscess a wall is thick to 2-4mm, with unclear contours and horizontal level of liquid.
For a tumour which disintegrates - a cavity of a wrong form, wall of different thickness, there is no liquid or it may be rarely.An important value has the state of pulmonary tissue, surrounding cavity: there are foci around at tuberculosis, a strengthening of a vascular pattern at an abscess, at an air cyst - a lung pattern is normal or impoverished.
Plural cavities can be at cystic disease, at abscess formation pneumonias and bronchoectasis.
Sometimes a bronkhography is used at bronchoectasis for clarification of diagnosis.
a 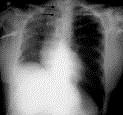 b
b 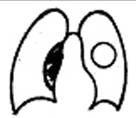 c
c 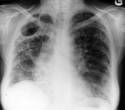
Fig.15.17. Spacious (pneumothorax) and limited (cavity) increase of lungs radiolucency
10. Spasious increase of lung’s radiolucency
Is observed both at an intrapulmonar process and at presence of air in a pleura cavity - pneumothorax. Pulmonary process can be limited (lobe or a few segments) at compensate hyperinflation (at atelectasis in contiguous lobes and segments) and widespread - at obstructive lung emphysema. The lung’s pattern becomes impoverished - less shallow vessels, the size of thorax increases, ribs are disposed horizontally in the superior departments of thorax, and the diaphragm goes down. At respiratory practically radiolucency does not change.
At pneumothorax a pulmonary collapse which slept is disponsed, in an uprooted department with an external clear contour, in intercostals spases lung pattern is not evident. Pneumatization of lungs can be observed at congenital hypoplasia of lungs.
Changes of diaphragmal shade and mediastinal organs position
Reason of pride of place of diaphragm cupula can be diaphragm relaxation as a result of paresis of diaphragm nerve, atelectasis or cirrhosis of lobe lungs, increases of liver, subdiaphragmal abscess, and ascites. A diaphragm occupies low position at emphysema, exudative pleurisy, and pneumothorax. Deformed diaphragm contour is through diaphragm hernia, pleura accretions, uneven reduction of parts of diaphragm muscle.
Displacements of the shade of mediastinal organs in a healthy side cause an exudative pleurisy, emphysema, partial pneumonia, mediastinal tumours, and in a side patology - cirrhosis, aplasy of the one lung.
Roentgeno-functional signs of thoracal organs state. The state of thoracal organs is studied in the process of respiratory, reductions of the heart, change of the body position and others like that. A respiratory function is estimated after the excursion of diaphragm, which can be normal (4-6 sm), megascopic, diminished, absent, paradoxical. Shade of pathological formation in lungs, related to the thorasic wall, moves upwards during inhalation and downward during exhalation, and intrapulmonal - vice versa, down at inhalation and up at exhalation. Shades of not dense formations (e.g. cysts, limited exudative pleurisy) some narrow in the moment of inhalation, and to exhalation -broaden.
1) Goltsnecht-Yakobson’s symptome is push-like displacement of mediastinum organs toward hypoventilasion or atelectasis during the forced inhalation;
2) Prozorov’s symptom is a displacement of mediastinal organs in a healthy side during the forced exhalation or couhg shove;
3) respirator emphysema`s symptome is saving of high radiolucency of lobe or segment after inhalation in the case of valvular mechanism of violation ventilation.
At sufficient pulmonary ventilation there is a substantial difference of the lungs radiolucency in the moment of maximal inhalation and exhalation (Falconi`s test). At emphysema, this difference will be little expressed.
At presence of free liquid in a pleura cavity there is its moving during examination sick in different positions: on the back, on the anterior, on a side.
An independent pulsation is incident to physiology (heart, aorta) and pathological formations (aneurysm of aorta, pulmonary artery, arteriovenous aneurysm). Pulsational transmission displacements look after physiology (to the esophagus) and pathological (cysts) formations which adjoin to the heart or aorta.
Radio diagnostics of the breathing organs inflammatory diseases.
Bronchitis
Bronchitis (see fig 16.1) is inflammation of bronches, which is clinically shown up by a cough with plenty of sputum, increase of the body temperature, stuffiness, and intoxication.
At an acute bronchitis a roentgenological pattern is inexpressive. Only in the case of heavy motion, strengthening of lung pattern is marked, sometimes visible dual strips of the thickened walls of bronches of the 3-4th orders and them U-like forks.
A chronic bronchitis is characterized by strengthening and deformation of lung pattern. The walls of bronches are thickened roentgenological determined as dual linear shades (symptom of "rails") and ring-shades in the case of axial location of bronches in anterior alion of x-ray irradiation. On bronchograma the inequality to the contour of bronches is noticeable, openings of mucus glands are extended, the amount of bronchial branches is diminished. Almost half of the patients with a chronic bronchitis have a normal roentgenological pattern, and pathological changes can appear through complication - pneumonia or emphysema.
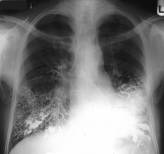
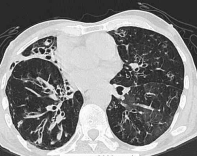
Fig.16.1. Bronkhoectasis is on a sciagram and CT
Pneumonia
Modern classification of pneumonias: 1) unhospital (domestic); 2) hospital (arises up through 48 hours after patient`s hospitalization); 3) aspirational; 4) for persons with an immunodeficiency.
Pneumonia is an inflammation of lungs with involvement in the inflammatory process of all of component parts of pulmonary tissue: bronches, bronchiols, alveoles, connecting tissue and other. Pneumonias classify on ethiology (bacterial, viral, mycotic), clinical motion (acute, chronic, atypicial), clinico-morphological description (lobar, segmentar, interstitial).
Acute pneumonia begins suddenly and shows up the increase of temperature of the body to 38-39°, by headache and pain in the thorax, which increase during a cough. A cough at first is dry, then moist. Wheezes and crepitation appear. In bloodwe can be seen hypergranulocytosis, increase of ESR, eosinophylia, and thrombocytopenia. Pathanatomichaly in the area of inflammatory infiltration, alveolus are filled with exudate.
Lobar (crupous) pneumonia in our time rarely will strike all of lobe and limited by 1-2 segments, that is why it is often named segmentary pneumonia. Roentgenological distinguish 3 stages of lobar pneumonia: wave, hepatisation and permitios.
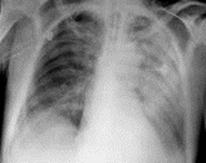
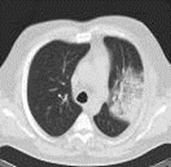
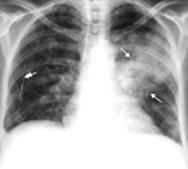
Fig.16.2 Crupous pneumonia is in the stage of hepatisation and permitios
In the stage of wave, that lasts about 1-2 days, there is a wave of blood in pulmonary vessels. There is strengthening of lung pattern in the area of defeat, root lungs is extended, without a clear structure, and the bulge of adjoining pleura appears in the case of subpleural location of pathological process. Stage of hepatisation, that lasts 3-9 days, characterizes the expressed inflammation with exudation of blood plasma rich on a fibrin to the alveoles, the thrombosis of small vessels and necrosis of pulmonary parenchym is possible. Roentgenological - homogeneous shade of the middle intensity appears with protuberant scopes. From the side of interlobar fissure shade has an even clear contour, because inflammation does not spread on surrounding lobes. At localization of pneumonia in the superior or middle lobe a low bound can be protuberant from the increase of volume and weight of lobe and its "sagging", or through the development of concomitant interlobar pleurisy. The image of air strips of forks bronches (symptom of "air bronchography") is saved, that facilitates differential diagnostics with and cancer of lungs. In the stage of permitios, that lasts usually 7-10 days, takes place dilution and proteolise of fibrin. Intensity of the homogeneous darkening diminishes roentgenological, beginning from superior and middle departments of the lobe. A lung pattern, extended and a root is unstructured lungs, is enriched, thickened an interlobar pleura can be observed yet during a month after convalescence.
Bronchopneumonia (see fig 16.3) is inflammation of separate pulmonary lobes and their groups, rarer acinus. More frequent all pneumonic hearths are disposed in inferior lobes, possibly in both lungs. Roentgenological observed calculation of focal shade of middle intensity with unclear contours, small or large sizes (micro- or macro-focal pneumonia) which quite often meet between it self, forming the whole areas of infiltration of considerable departments of segment or lobe (pneumonia with confluent foci). At the level focal shades a lung pattern is washed out, root lungs infiltrated. Typical for focal pneumonias is a rapid changeability of roentgenological pattern: during 4-6 days symptoms grow, and in 10-12 days of hearth resolve fully. The bronchopneumonia, as a rule, is develops from bronchitis, when an inflammatory process from bronches spread to pulmonary parenchyma and focal shades disposes after bronchial motion.
Interstitial pneumonia is caused by various viruses. Endothelial of capillaries and interstitial tissue, which surrounds vessels, bronches, acinuses is struck. Clinically shows up intoxication (headache, cold, cough, and feverish state), stuffiness, and cyanosis. Physical changes are not expressed: percution of changes are not discovered, auscultation - hearkened unset, fine moist and dry rales. Roentgenological in lungs from one or both sides there are focal shades of different size with different contours, strengthening and deformation of lung pattern, the structure of root diminishes. As a result of joining of bacterial infection in parenchym there are infiltrative changes on the type of micro-focal pneumonia. Such mixed interstitial parenchymatous pneumonia has the protracted motion - to 2 months.
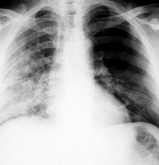
Fig.16.3 Bronchpneumonia
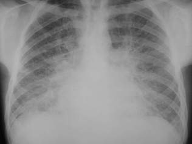
Fig.16.4. interstitial pneumonia
It is possible to define localization and prevalence of process more precisely by computer tomography before the changes of pulmonary tissue appear at acute pneumonia.
The pneumonia complicated by an abscess (see fig 16.5)- festering inflammation of pulmonary tissue and its disintegration with formation of cavity which arises up usually in 2-3 weeks from the beginning of acute pneumonia. In motion of acute abscess distinguish 3 stages: 1) festering infiltration and forming of festering cavity, when intensity of shade of acute pneumonia grows roentgenological, and its contours are round; 2) emptying (drainage)of the festering cavity through a bronchus, when roentgenological ring-shade of abscess appears with a thick wall and horizontal level of liquid; 3) absorbtion and scarring, when the thickness of wall of abscess diminishes, the cavity of abscess acquires extended, later fissural forms and in 2-3 months is substituted by a scar.
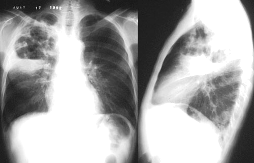
Fig.16.5. Pneumonia complicated by an abscess
Date: 2014-12-28; view: 3633
| <== previous page | | | next page ==> |
| Miliary Pattern | | | Pleurisy |