
CATEGORIES:
BiologyChemistryConstructionCultureEcologyEconomyElectronicsFinanceGeographyHistoryInformaticsLawMathematicsMechanicsMedicineOtherPedagogyPhilosophyPhysicsPolicyPsychologySociologySportTourism
Legs shape: X- and O-shaped legs.
Heel shape deformation: internal or external calcaneal bone deviation.
Varicosity of veins.
3 was admitted as the critical level of connective tissue structure lesion phenotypic signs allowing to consider a teen a person with connective tissue dysplasia. [ 3,8,10,13]. Cases in which the external dysplasia phenotypic signs didn’t match the connective tissue heart carcass dysplastic changes were excluded from the analysis.
Summary: analysis of sports injuries in 971 athletes of different kinds of sports with musculoskeletal system connective tissue dysplasia phenotypic symptoms complexes, 45 of which were basketball, volleyball and rowing national team athletes was made. The frequency of injuries depended not only on the specifics of sports activity, but on the presence of connective tissue dysplasia signs too. The reliable frequency of injuries increasing in persons with connective tissue dysplasia: 2,5 times more often in national basketball team and 2 times more often in volleyball. The obtained data testify the necessity of connective tissue dysplasia signs registration to cure and prevent the sports injuries etiologically and pathogenetically.
Key words: sports, sports injury, connective tissue dysplasia, musculoskeletal system connective tissue dysplasia, mutation of genes.
Chronic and acute injuries are always important issues for athletes, because the results of that injuries can influence the whole career or the sports longevity significantly. The main injury causes are considered to be:
А. Methodical causes:
1. Sports training principals noncompliance: continuity, cyclicity, workload progressive increasing.
2. Overwork practices.
3. Backbreaking, unfamiliar, difficult exercises.
4. Practice without warm-up or with insufficient warm-up.
5. Lack of athlete’s concentration.
Б. Organizational causes:
- Qualification of the coach.
- Not paying attention to sex, age and physical conditions in groups staffing.
- Safety tools absence, “strong vs weak” exercises, etc.
- Too much people in a group.
- Training without a coach, at a low temperature conditions.
- Athletes allowance to practice without previous medical exam; early returning to training after illness or injury; hygiene procedures incompliance.
- Non-appropriate training places conditions (bad illumination, insufficient ventilation, low quality surface, irrational equipment location, etc.).
- Sports discipline and regime disturbance.
Not diminishing the significance of these factors, we found another ones causing athlete’s musculoskeletal injuries. It is well known that the cause of connective tissue dysplasia development is genes responsible for connective tissue extracellular matrix components synthesis or decay mutation. [6]. Nowadays a big group of myogenic connective tissue dysplasia conjugated with mutation of extracellular matrix protein genes (collagen of different, fibrillin, tenaskin), growth factors receptors genes, particularly TGF-β (transforming growth factor-β), and matrix metalloproteinase [4,5,6,7,10,11,12,13] is identified. Thus connective tissue and dysplastic process in it form defective carcass (joint surfaces of bones, covering joint cartilages, disc and ligaments), moved by muscles with normal anlage. There is a dissociation between muscle contractions strength and impaired elastic and tension characteristics of a joint leading to connective tissue joint elements lesion: ligaments and disk, during ordinary functional workload. Tissue anatomic structure or an organ lesion [2,8] develops under an influence of physical (mechanical and thermal) injuring factors, under which force excesses tissue strength; areas of functional and trophic lesions common signs of which are dystrophy and aseptic inflammation form in different parts of musculoskeletal system. This functional lesions are musculoskeletal system chronic overuse signs. Acute injuries (muscle micro-injuries, tendon and ligament tears, etc.), are considered to be the musculoskeletal system chronic lesion complications.
Research task – to find out how much the connective tissue dysplasia influences the sports injuries frequency.
After the clinical part of work in which the external phenotypic stigmas of the musculoskeletal system development were found out, the most often registered connective tissue dysplasia signs were compared in control group of athletes and three national selection teams (table №1,2; diagram №1).
Connective tissue dysplasia signs presence in athletes ( % ). Table №1
| Connective tissue dysplasia signs | Control group n= 971 | Basketball team n=14 | Rowing team n =11 | Volleyball team n =20 |
| Bad posture | 46,0 | 57,1 | 27,3 | 45,0 |
| Asthenic type of constitution | 36,1 | 71,4 | 9,1 | 70,0 |
| Flat-footedness: -longitudinal -transversal | 17,3 13,9 3,4 | 32,9 25,7 7,2 | 18,2 18,2 - | 30,0 19,7 10,3 |
| Joints hypermobility: -hand fingers overextension -elbow joints overextension -knee joints overextension | 8,3 3,6 2,9 1,8 | 35,7 21,4 7,15 7,15 | 9,1 9,1 | 70,0 35,7 23,3 11,0 |
| Skin hyper-extensibility | 13,5 | 35,7 | 9,1 | 25,0 |
Obtained data indicate that connective tissue dysplasia signs are seen more often in basketball and volleyball players than in rowers.
Basketball, volleyball and rowing athletes connective tissue dysplasia signs comparative analysis (%). (Diagram №1).
Diagram №1
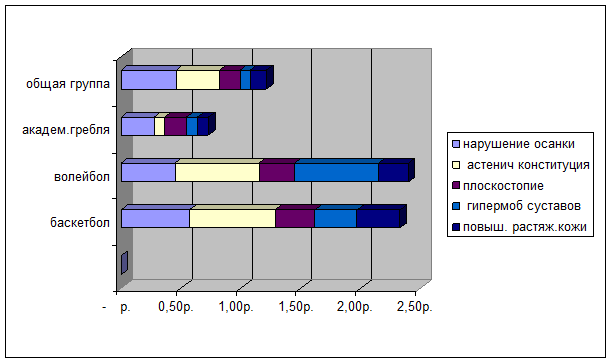
We were interested in connective tissue dysplasia signs influence on the frequency of musculoskeletal system injuries degree.
The musculoskeletal system diseases and injuries frequency and a character in basketball and volleyball were analyzed as these teams had shown the majority of connective tissue dysplasia signs.
Obtained musculoskeletal injuries in basketball and volleyball players with and without connective tissue dysplasia signs analysis data is represented in Table №2.
Musculoskeletal injuries registration frequency in basketball and volleyball players with and without connective tissue dysplasia signs.
Таблица 2
| Injury character | Basketball With CTD Without CTD % N=14 | Volleyball With CTD Without CTD % N=20 |
| 1. Deltoid ligament of ankle sprains | 35.7 14.3 | 20.0 10.0 |
| 2. Wrist ligaments sprain | 7.1 - | 15.0 5.0 |
| 3. Hand fingers dislocations | - - | 10.0 5.0 |
| 4. Anterior hip sprains | - - | 5.0 - |
| 5. Rotator cuff injuries | 7.1 - | 20.0 10.0 |
| 6 .Achilles tendon tendinitis | 71.4 50.0 | 5.0 - |
| 7. Lumbosacral spine dystrophic and degenerative changes | 85.7 35.7 | 75.0 30.0 |
| 8. Meniscus injuries | 35.7 14.3 | 5.0 - |
| 9.Abdominal muscles sprains | - 7.1 | 5.0 - |
| 10.Medial collateral ligament of knee sprain | 85.7 28.6 | 5.0 - |
| 11.Knee osteoarthritis | 64.3 35.7 | 75.0 20.0 |
| 12."Jumper’s knee" | 50.0 21.4 | 10.0 - |
The obtained data analysis indicated that the frequency of injuries depended not only on the sports activity specifics – the rotator cuff and wrist ligaments sprains were registered more often in volleyball players, but on the presence of connective tissue dysplasia signs as well. Musculoskeletal system lesions were registered two times more often in volleyball players with connective tissue dysplasia signs than in those without. (Diagram №2)
Diagram №2
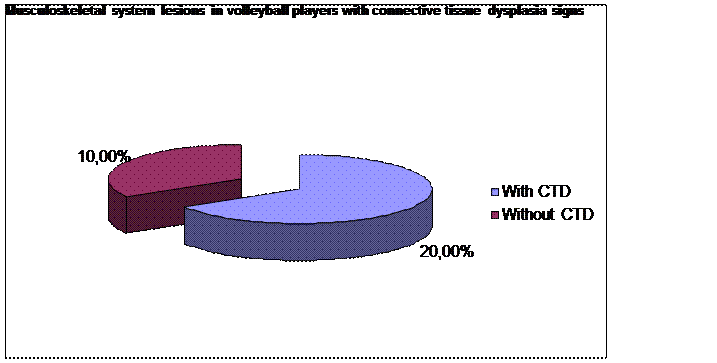
Medial collateral ligament of the knee sprains, Achilles tendon tendinitis, meniscus injuries and a “jumper’s knees” were registered in basketball players. Ankle ligaments sprains were the most frequent injuries in athletes with connective tissue dysplasia in both teams, which matches the National College Athletes Association data (NCAA) [12].
Concerning the musculoskeletal system chronic conditions, it should be noted that the lumbosacral spine dystrophic and degenerative changes and the knee osteoarthritis were registered in both groups of athletes with high frequency.
Concerning basketball players with connective tissue dysplasia, it should be noted that the musculoskeletal system injuries were registered 2,5 times more often than in players without connective tissue dysplasia. (Diagram №3)
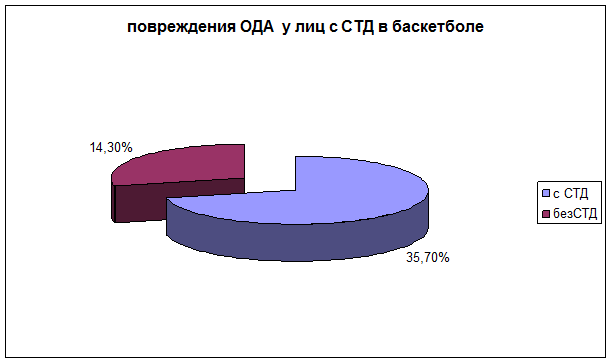
Athletes were analyzed biochemically. It allowed to estimate the connective tissue metabolism, confirm the diagnosis and predict condition progress. Oxyproline and glycosaminoglycans were detected in daily urine, as well as lysine, proline and oxyproline in blood serum [4,5,6,7]. Athletes were rehabilitated by means of psychotherapy and physiotherapy, and for pathogenetic base of connective tissue inconsistency the collagen metabolism lesion correction was made. Athletes were given collagen production stimulators, ascorbic acid, mucopolysaccharides (chondroitin sulfate, glucosamine sulfate), vitamins of a B group (В1, В2, В3, В6) and minerals (cuprum, zinc, magnesium), as they are intra- and extracellular collagen molecule and other connective tissue structural elements maturation cofactors. [3,7]. Magnesium played a special role, as under it’s deficiency collagen and elastin fibers, hyaluran polysaccharide filaments degeneration, increasing of the amount of dysfunctional t-RNA molecules took place, thus decreasing the protein synthesis speed [13].
Conclusion:
1. Obtained data indicates that the frequency of injuries in athletes depends not only on sports activity specifics, but on the presence of connective tissue dysplasia signs as well.
In athletes with connective tissue dysplasia signs definitely more than two times often occur musculoskeletal injuries, than in athletes without them, the majority of injuries were ligaments sprains, tears and ruptures.
2. According to contemporary sports traumatology conception, connective tissue dysplasia signs should be taken into account while rehabilitating an athlete.
The following procedures should be included:
1. Injury relapse prevention.
2. P.R.I.C.E. protocol (P- Protect; R-Rest; I- Ice; C-Compression; E-Elevation).
3. Early mobilization and full range of motion restoration.
4. Balance, strength and endurance restoration.
5. Appropriate physical load for cardiovascular system functional condition impairment.
6. Proprioception, balance, agility, flexibility.
7. Taping, kinesio-taping and supporting tools.
8. Psychological help.
9. Progressive functional rehabilitation program.
10. Medicamental treatment.
Literature.
11.Beighton P., De Paepe A., Steinmann B. et al. Ehlers-Danlos syndromes: revised nosology, Villefranche, 1997. Ehlers-Danlos National Foundation (USA) and EhlersDanlos Support Group (UK). Am JMed Genet 1998;77(1): 31–7.
12 Hootman J.M., Dick R., Agel J. Epidemiology of Collegiate Injuries for 15 Sports: Summary and Recommendations for Injury Prevention Initiatives J Athl Train. 2007, vol.42, N.2, pp.311–319 [PDF]
13. Glesby M. J., Pyeritz R.E. Association of mitral valve prolapse and systemic abnormalities of connective tissue. A phenotypic continuum // JAMA – 1989. – Vol.262. – P.523 – 528.
14.Grahame R. Joint hypermobility and genetic collagen disorders: are they related? Arch Dis Child 1999; 80(2):188–91.
15Grahame R., Bird H.A., Child A. The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome (BJHS). J Rheumatol 2000;27(7): 1777–9.
16 Kirk J.A., Ansell B.M., Bywaters E.G. The hypermobility syndrome. Musculoskeletal complaints associated with generalized joint hypermobility. Ann Rheum Dis 1967;26(5):419–25.
17. Zweers M.C., Bristow J., Steijlen P.M. et al. Haploinsufficiency of TNXB is associated with hypermobility type of Ehlers-Danlos syndrome. AmJHumGenet 2003; 73(1):214–17.
18.Sillence D.O., Rimoin D.L. Classification of osteogenesis imperfect. Lancet 1978;1(8072):1041–2.
19. SimpsonM.R. Benign joint hypermobility syndrome: evaluation, diagnosis, and management. J Am Osteopath Assoc 2006; 106(9): 531-6.
Information about authors:
- mrs. Tatiana Gurevich - PhD in medical sciences, AP of the department of physical methods of treatment and sports medicine in Saint-Petersburg State Medical University named after I. P. Pavlov
Cell phone: +7(812)998-68-20, е-mail: tatyana_gurevich@ mail.ru
2. mr. Kirill Konovalenko, MD, sports medical doctor in Saint-Petersburg volleyball team
Cell phone: +7-905-588-08-35, e-mail: dominator39@mail.ru
3. mr. Dmitriy Kirillov - PhD in medical sciences, Saint-Petersburg “Sestroretskiy sanatoriy” sanitarium CFO
Cell phone: +7- 951-689-74-45 e-mail: kd_dok@mail.ru
4. mr. Pavel Mustaphin -
5. mr. Valeriy Kozlov - head of NORTH EUROPEAN INSTITUTE of SPORTS METHODOLOGY and MEDICAL BIOLOGY, Estonia
e-mail: valeriy.kozlow@gmail.com
Date: 2015-01-12; view: 2210
| <== previous page | | | next page ==> |
| The research objective was to study connective tissue dysplasia interrelation with injuries in athletes during practices and competitions. | | | CULTURAL DIFFERENCES |