
CATEGORIES:
BiologyChemistryConstructionCultureEcologyEconomyElectronicsFinanceGeographyHistoryInformaticsLawMathematicsMechanicsMedicineOtherPedagogyPhilosophyPhysicsPolicyPsychologySociologySportTourism
АМмЙАжDVT, Jeep venous [Ы)ЫкРЕ, pulmonary embolism. 3 page
A. Ampicillin, 500 mg IV q6h
B. Ceftriaxone, 1 g IV q24h
C. Endotracheal intubation and ampicillin, 500 mg IV q6h
D. Endotracheal intubation, 1 g IV q24h of ceftriaxone, and 600 mg IV q6h of clindamycin
E. Laryngoscopy and close observation
IV-77. All of the following statements regarding Moraxella catarrhalis as an upper respiratory pathogen are true EXCEPT:
A. Clinical features allow distinction between COPD exacerbations caused by M. catarrhalis and
H. influenzae.
B. It causes otitis media in children.
C. It is the second most common bacterial cause of COPD exacerbations.
D. Most strains are susceptible to azithromycin.
E. Most strains express β-lactamase activity.
IV-78. A 75-year-old patient presents with fevers and wasting. He describes fatigue and malaise over the past several months and is concerned that he has been losing weight. On examination, he is noted to have a low-grade fever, and a soft diastolic heart murmur is appreciated. Laboratory tests reveal a normocytic, normochromic anemia. Three separate blood cultures grow Cardiobacterium hominis. Which of the following statements is true about this patient’s clinical condition?
A. Antibiotics are not likely to improve his condition.
B. Echocardiography findings will likely be normal.
C. He has a form of endocarditis with a high risk of emboli.
D. He will likely need surgery.
E. The positive blood culture results are likely because of a skin contaminant.
IV-79. A 38-year-old woman with frequent hospital admissions related to alcoholism comes to the emergency department after being bitten by a dog. There are open wounds on her arms and right hand that are purulent and have necrotic borders. She is hypotensive and is admitted to the intensive care unit. She is found to have disseminated intravascular coagulation and soon develops multiorgan failure. Which of the following is the most likely organism to have caused her rapid decline?
A. Aeromonas spp.
B. Capnocytophaga spp.
C. Eikenella spp.
D. Haemophilus spp.
E. Staphylococcus spp.
IV-80. A 56-year-old man with a history of hypertension and cigarette smoking is admitted to the intensive care unit after 1 week of fever and nonproductive cough. Imaging shows a new pulmonary infiltrate, and urine antigen test result for Legionella is positive. Each of the following is likely to be an effective antibiotic EXCEPT:
A. Azithromycin
B. Aztreonam
C. Levofloxacin
D. Tigecycline
E. Trimethoprim/sulfamethoxazole
IV-81. All of the following are risk factors for the development of Legionella pneumonia EXCEPT:
A. Glucocorticoid use
B. HIV infection
C. Neutropenia
D. Recent surgery
E. Tobacco use
IV-82. A 72-year-old woman is admitted to the intensive care unit with respiratory failure. She has fever, obtundation, and bilateral parenchymal consolidation on chest imaging. Which of the following is true regarding the diagnosis of Legionella pneumonia?
A. Acute and convalescent antibodies are not helpful because of the presence of multiple serotypes.
B. Legionella can never be seen on a Gram stain.
C. Legionella cultures grow rapidly on the proper media.
D. Legionella urinary antigen maintains utility after antibiotic use.
E. Polymerase chain reaction for Legionella DNA is the “gold standard” diagnostic test.
IV-83. An 18-year-old man seeks attention for a severe cough. He reports no past medical history and excellent health. Approximately 7 days ago, he developed an upper respiratory syndrome with low-grade fever, coryza, some cough, and malaise. The fever and coryza has improved, but over the past 2 days, he has had an episodic cough that often is severe enough to result in vomiting. He reports receiving all infant vaccinations but only tetanus in the past 12 years. He is afebrile, and while not coughing, his chest examination is normal. During a coughing episode, there is an occasional inspiratory whoop. Chest radiography findings are unremarkable. Which of the following is true regarding his likely illness?
A. A fluoroquinolone is recommended therapy.
B. Cold agglutinin results may be positive.
C. Nasopharyngeal aspirate for DNA testing is likely to be diagnostic.
D. Pneumonia is a common complication.
E. Urinary antigen testing results remain positive for up to 3 months.
IV-84. Which of the following is the most common cause of traveler’s diarrhea in Latin America?
A. Campylobacter jejuni
B. Entamoeba histolytica
C. Enterotoxigenic Escherichia coli
D. Giardia lamblia
E. Vibrio cholerae
IV-85. In the inpatient setting, extended-spectrum β-lactamase (ESBL)–producing gram-negative infections are most likely to occur after frequent use of which of the following classes of antibiotics?
A. Carbapenems
B. Macrolides
C. Quinolones
D. Third-generation cephalosporins
IV-86. A 25-year-old woman presents to the clinic complaining of several days of worsening burning and pain with urination. She describes an increase in urinary frequency and suprapubic tenderness but no fever or back pain. She has no past medical history with the exception of two prior episodes similar to this in the past 2 years. Urinalysis shows moderate white blood cells. Which of the following is the most likely causative agent of her current symptoms?
A. Candida spp.
B. Escherichia coli
C. Enterobacter spp.
D. Klebsiella spp.
E. Proteus spp.
IV-87. All of the following statements regarding intestinal disease caused by strains of Shiga toxin– producing and enterohemorrhagic E. coli are true EXCEPT:
A. Antibiotic therapy lessens the risk of developing hemolytic uremic syndrome.
B. Ground beef is the most common source of contamination.
C. Gross bloody diarrhea without fever is the most common clinical manifestation.
D. Infection is more common in industrialized than developing countries.
E. O157:H7 is the most common serotype.
IV-88. A 63-year-old man has been in the ICU for 3 weeks with slowly resolving ARDS after an episode of acute pancreatitis. He remains on mechanical ventilation through a tracheostomy. Over the past week, he has had gradual lessening of his mechanical ventilator needs and slight improvement of his radiograph. He has been afebrile with a normal WBC for the past 10 days. Over the past 24 hours, his FiO2 has been increased from 0.60 to 0.80 to maintain adequate oxygenation. In addition, he has
developed newly purulent sputum with a right lower lobe infiltrate, fever to 101.5°C, and a rising WBC. Sputum gram stain shows gram-negative plump coccobacilli that are identified as Acinetobacter baumannii. All of the following are true about this organism EXCEPT:
A. Mortality from bloodstream infection approaches 40%.
B. Multidrug resistance is characteristic.
C. They are a growing cause of hospital-acquired pneumonia and bloodstream infections in the
United States.
D. They are not yet a significant problem in Asia or Australia.
E. Tigecycline is treatment of choice for bloodstream infection.
IV-89. Helicobacter pylori colonization increases the odds ratio of developing all of the following conditions EXCEPT:
A. Duodenal ulcer disease
B. Esophageal adenocarcinoma
C. Gastric adenocarcinoma
D. Gastric mucosa-associated lymphoid tissue (MALT) lymphoma
E. Peptic ulcer disease
IV-90. One month after receiving a 14-day course of omeprazole, clarithromycin, and amoxicillin for Helicobacter pylori–associated gastric ulcer disease, a 44-year-old woman still has mild dyspepsia and pain after meals. What is the appropriate next step in management?
A. Empirical long-term proton pump inhibitor therapy
B. Endoscopy with biopsy to rule out gastric adeno-carcinoma
C. H. pylori serology testing
D. Second-line therapy for H. pylori with omeprazole, bismuth subsalicylate, tetracycline, and
metronidazole
E. Urea breath test
IV-91. In the developed world, seroprevalence of Helicobacter pylori infection is currently
A. Decreasing
B. Increasing
C. Staying the same
D. Unknown
IV-92. A 42-year-old man with heme-positive stools and a history of epigastric pain is found to have a duodenal ulcer that is biopsy-proven positive for H. pylori. All of the following are effective eradication regimens EXCEPT:
A. Amoxicillin and levofloxacin for 10 days
B. Omeprazole, clarithromycin, and metronidazole for 14 days
C. Omeprazole, clarithromycin, and amoxicillin for 14 days
D. Omeprazole, bismuth, tetracycline, and metronidazole for 14 days
E. Omeprazole and amoxicillin for 5 days followed by omeprazole, clarithromycin, and tinidazole
for 5 days
IV-93. A sputum culture from a patient with cystic fibrosis showing which of the following organisms has been associated with a rapid decline in pulmonary function and a poor clinical prognosis?
A. Burkholderia cepacia
B. Pseudomonas aeruginosa
C. Staphylococcus aureus
D. Staphylococcus epidermidis
E. Stenotrophomonas maltophilia
IV-94. Which single clinical feature has the most specificity in differentiating Pseudomonas aeruginosa sepsis from other causes of severe sepsis in a hospitalized patient?
A. Ecthyma gangrenosum
B. Hospitalization for severe burn
C. Profound bandemia
D. Recent antibiotic exposure
E. Recent mechanical ventilation for >14 days
IV-95. All of the following agents may be effective when used as monotherapy in a nonneutropenic patient with Pseudomonas aeruginosa bacteremia EXCEPT:
A. Amikacin
B. Cefepime
C. Ceftazidime
D. Meropenem
E. Piperacillin/tazobactam
IV-96. Five healthy college roommates develop a rapid (<8 hours) onset of abdominal pain, cramping, fever to 38.5°C, vomiting, and copious nonbloody diarrhea while camping. They immediately return for hydration and diagnosis. A stool culture grows Salmonella enteritidis. All of the statements regarding their clinical syndrome are true EXCEPT:
A. Antibiotic therapy is not indicated.
B. Bacteremia occurs in fewer than 10% of cases.
C. The most likely source was undercooked eggs.
D. There is no vaccine available for this illness.
E. They have enteric (typhoid) fever.
IV-97. Two days after returning from a trip to Thailand, a 36-year-old woman develops severe crampy abdominal pain, fever to 40°C, nausea, and malaise. The next day, she begins having bloody mucopurulent diarrhea with worsening abdominal pain and continued fever. She reports she was in Bangkok during monsoonal flooding and ate fresh food from stalls. A stool examination shows many neutrophils, and culture grows Shigella flexneri. Which of the following statements regarding her clinical syndrome is true?
A. An effective vaccine for travelers is available.
B. Antibiotic therapy prolongs the carrier state and should not be administered unless she develops
bacteremia.
C. Antimotility agents are effective in reducing the risk of dehydration.
D. Ciprofloxacin is recommended therapy.
E. Her disease can be distinguished from illness caused by Campylobacter jejuni on clinical
grounds by the presence of fever.
IV-98. A previously healthy 32-year-old graduate student at the University of Wisconsin describes 1 to 2 days of fever, myalgia, and headache followed by abdominal pain and diarrhea. He has experienced up to 10 bowel movements over the past day. He has noted mucus and blood in the stool. The patient notes that 3 days ago, he was at a church barbecue, where several people contracted a diarrheal illness. He has not traveled in more than 6 months and has no history of GI illness. Physical examination is unremarkable except for a temperature of 38.8°C and diffuse abdominal tenderness. Laboratory findings are notable only for a slightly elevated leukocyte count and an elevated erythrocyte sedimentation rate. Wright’s stain of a fecal sample reveals the presence of neutrophils. Colonoscopy reveals inflamed mucosa. Biopsy of an affected area discloses mucosal infiltration with neutrophils, monocytes, and eosinophils; epithelial damage, including loss of mucus; glandular degeneration; and crypt abscesses. Which of the following microbial pathogens is most likely to be responsible for his illness?
A. Campylobacter
B. Escherichia coli
C. Norwalk agent
D. Rotavirus
E. Staphylococcus aureus
IV-99. In the patient described in question IV-98, which of the following is recommended therapy?
A. Azithromycin
B. Ceftriaxone
C. Lomotil only for symptoms
D. Metronidazole
E. Tinidazole
IV-100. While working for a relief mission in Haiti, you are asked to see a 19-year-old patient with profuse watery diarrhea as shown in Figure IV-100. The patient is mildly hypotensive and tachycardic and is afebrile. There is no abdominal tenderness. All of the statements regarding this patient’s illness are true EXCEPT:

FIGURE IV-100 (see Color Atlas)
A. Antibiotic therapy shortens the duration of disease and hastens clearance of the organism from
stool.
B. Morbidity or death is mediated by bacteremia and multiorgan failure.
C. Point of care antigen testing is available.
D. The diarrhea is toxin mediated.
E. Vaccines with moderate efficacy are available outside the United States.
IV-101. A 45-year-old man from western Kentucky presents to the emergency department in September complaining of fevers, headaches, and muscle pains. He recently had been on a camping trip with several friends during which they hunted for their food, including fish, squirrels, and rabbits. He did not recall any tick bites during the trip but does recall having several mosquito bites. For the past week, he has had an ulceration on his right hand with redness and pain surrounding it. He also has noticed some
pain and swelling near his right elbow. None of the friends he camped with have been similarly ill. His vital signs are blood pressure of 106/65 mmHg, heart rate of 116 beats/min, respiratory rate of 24 breaths/min, and temperature of 38.7°C. His oxygen saturation is 93% on room air. He appears mildly tachypneic and flushed. His conjunctiva are not injected, and his mucous membranes are dry. The chest examination reveals crackles in the right mid-lung field and left base. His heart rate is tachycardic but regular. There is a II/VI systolic ejection murmur heard best at the lower left sternal border. His abdominal examination is unremarkable. On the right hand, there is an erythematous ulcer with a punched-out center covered by a black eschar. He has no cervical lymphadenopathy, but there are markedly enlarged and tender lymph nodes in the right axillae and epitrochlear regions. The epitrochlear node has some fluctuance with palpation. A chest radiograph shows fluffy bilateral alveolar infiltrates. Over the first 12 hours of his hospitalization, the patient becomes progressively hypotensive and hypoxic, requiring intubation and mechanical ventilation. What is the most appropriate therapy for this patient?
A. Ampicillin, 2 g IV q6h
B. Ceftriaxone, 1 g IV daily
C. Ciprofloxacin, 400 mg IV twice daily
D. Doxycycline, 100 mg IV twice daily
E. Gentamicin, 5 mg/kg twice daily
IV-102. A 35-year-old man comes to the emergency department complaining of an acute-onset high fever, malaise, and a tender lymph node. The patient returned from a camping trip in the Four Corners region of the United States (junction area of New Mexico, Arizona, Colorado, and Utah) 4 days ago and reports being bitten by fleas. He has no past medical history and works as a university professor. He denies illicit drug use. On physical examination, he is lethargic but oriented and has a temperature 39.4°C, heart rate of 105 beats/min, and blood pressure of 100/65 mmHg. There are numerous crusted flea bites on the upper legs. In the right inguinal region, there is an exquisitely tender 3- to 4-cm tense lymph node with surrounding edema but no lymphangitis. An aspirate of the node reveals small gram-negative coccobacilli that appear bipolar on Wright’s stain. Which of the following is the most likely causative organism?
A. Bartonella henselae
B. Epstein-Barr virus
C. Rickettsia rickettsia
D. Staphylococcus aureus
E. Yersinia pestis
IV-103. In the patient in question IV-102, which of the following therapeutic options is recommended?
A. Azithromycin
B. Gentamicin
C. No therapy; it is a self-limited disease
D. Vancomycin
E. Voriconazole
IV-104. A 24-year-old man with advanced HIV infection presents to the emergency department with a tan
painless nodule on the lower extremity (see Figure IV-104). He is afebrile and has no other lesions. He does not take antiretroviral therapy, and his last CD4+ T-cell count was 20/μL. He lives with a friend who has cats and kittens. A biopsy shows lobular proliferation of blood vessels lined by enlarged endothelial cells and a mixed acute and chronic inflammatory infiltrate. Tissue stains show gram-negative bacilli. Which of the following is most likely to be effective therapy for the lesion?
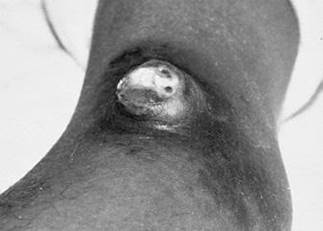
FIGURE IV-104 (see Color Atlas)
A. Azithromycin
B. Cefazolin
C. Interferon-α
D. Penicillin
E. Vancomycin
IV-105. A 38-year-old homeless man presents to the emergency department with a transient ischemic attack characterized by a facial droop and left arm weakness lasting 20 minutes and left upper quadrant pain. He reports intermittent subjective fevers, diaphoresis, and chills for the past 2 weeks. He has had no recent travel or contact with animals. He has taken no recent antibiotics. Physical examination reveals a slightly distressed man with disheveled appearance. His temperature is 38.2°C, heart rate is 90 beats/min, and blood pressure is 127/74 mmHg. He has poor dentition. Cardiac examination reveals an early diastolic murmur over the left third intercostal space. His spleen is tender and 2 cm descended below the costal margin. He has tender painful red nodules on the tips of the third finger of his right hand and on the fourth finger of his left hand that are new. He has nits evident on his clothes consistent with body louse infection. White blood cell count is 14,500/μL, with 5% band forms and 93% polymorphonuclear cells. Blood cultures are drawn followed by empirical vancomycin therapy. These culture results remain negative for growth 5 days later. He remains febrile but hemodynamically stable but does develop a new lesion on his toe similar to those on his fingers on hospital day 3. A transthoracic echocardiogram reveals a 1-cm mobile vegetation on the cusp of his aortic valve and moderate aortic regurgitation. A CT scan of the abdomen shows an enlarged spleen with wedge-shaped splenic and renal infarctions. What test should be sent to confirm the most likely diagnosis?
A. Bartonella serology
B. Epstein-Barr virus heterophile antibody
C. HIV polymerase chain reaction
D. Peripheral blood smear
E. Q fever serology
IV-106. A 26-year-old female college student presents with tender epitrochlear and axillary tender, firm, 3-cm lymph nodes on her left side. She has a 0.5-cm painless nodule on her left second finger. She reports low-grade fever and malaise over 2 weeks. She enjoys gardening and exotic fish collecting and owns several pets, including fish, kittens, and a puppy. She is sexually active with one partner. She traveled extensively throughout rural Southeast Asia 2 years before her current illness. The differential diagnosis includes all of the following EXCEPT:
A. Bartonella henselae infection
B. Lymphoma
C. Sporothrix schenckii infection
D. Staphylococcal infection
IV-107. A 24-year-old man seeks evaluation for painless penile ulcerations. He noted the first lesion about 2 weeks ago, and since that time, two adjacent areas have also developed ulceration. He states that there has been blood staining his underwear from slight oozing of the ulcers. He has no past medical history and takes no medication. He returned 5 weeks ago from a vacation in Brazil, where he did have unprotected sexual intercourse with a local woman. He denies other high-risk sexual behaviors and has never had sex with prostitutes. He was last tested for HIV 2 years ago. He has never had a chlamydial or gonococcal infection. On examination, there are three well-defined red, friable lesions measuring 5 mm or less on the penile shaft. They bleed easily with any manipulation. There is no pain with palpation. There is shotty inguinal lymphadenopathy. On biopsy of one lesion, there is a prominent intracytoplasmic inclusion of bipolar organisms in an enlarged mononuclear cell. Additionally, there is epithelial cell proliferation with an increased number of plasma cells and few neutrophils. A rapid plasma reagin test result is negative. Cultures grow no organisms. What is the most likely causative organism?
A. Calymmatobacterium granulomatis (donovanosis)
B. Chlamydia trachomatis (lymphogranuloma venereum)
C. Haemophilus ducreyi (chancroid)
D. Leishmania amazonensis (cutaneous leishmaniasis)
E. Treponema pallidum (secondary syphilis)
IV-108. A 35-year-old man is seen 6 months after a cadaveric renal allograft. The patient has been on azathioprine and prednisone since that procedure. He has felt poorly for the past week with fever to 38.6°C (101.5°F), anorexia, and a cough productive of thick sputum. Chest radiography reveals a left lower lobe (5-cm) mass with central cavitation. Examination of the sputum reveals long, crooked, branching, beaded gram-positive filaments. The most appropriate initial therapy would include the administration of which of the following antibiotics?
A. Ceftazidime
B. Erythromycin
C. Penicillin
D. Sulfisoxazole
E. Tobramycin
IV-109. A 67-year-old woman with a history of systemic hypertension presents to her local emergency department with 2 weeks of right jaw pain that now has developed an area of purulent drainage into her mouth. She reports an accompanying fever. She denies recent dental work. Aside from osteoporosis, she is healthy. Her only medications are alendronate and lisinopril. Physical examination is notable for a temperature of 101.1°F, right-sided facial swelling, diffuse mandibular tenderness, and an area of yellow purulent drainage through the buccal mucosa on the right side. Microscopic examination of the purulent secretions is likely to show which of the following?
A. Auer rods
B. Sialolith
C. Squamous cell carcinoma
D. Sulfur granules
E. Weakly acid-fast branching, beaded filaments
IV-110. In the patient described above, what is the most appropriate therapy?
A. Amphotericin B
B. Itraconazole
C. Penicillin
D. Surgical debridement
E. Tobramycin
IV-111. A 68-year-old homeless man with a long history of alcohol abuse presents to his primary care physician with several weeks of fever, night sweats, and sputum production. He denies nausea, vomiting, and other gastrointestinal symptoms. Examination is notable for a low-grade temperature, weight loss of 15 lb since the previous visit, and foul breath but is otherwise normal. Blood work, including complete blood count and serum chemistries, is unremarkable. A PPD is placed, and the result is negative. His chest radiograph is shown in Figure IV-111 . Which of the following is appropriate as initial therapy?

FIGURE IV-111
A. Bronchoscopy with biopsy of the cavity to diagnose squamous cell lung cancer
B. Esophagogastroduodenoscopy to diagnose hiatal hernia with aspiration
C. Immediate hospitalization and isolation to prevent spread of mycobacterium tuberculosis
D. Intravenous ceftriaxone and azithromycin for aspiration pneumonia
E. Oral clindamycin for lung abscess
IV-112. Which of the following is a major reservoir for anaerobic organisms in the human body?
A. Duodenum
B. Female genital tract
C. Gallbladder
D. Lung
E. Prostate
IV-113. All of the following factors influence the likelihood of transmitting active tuberculosis EXCEPT:
A. Duration of contact with an infected person
B. Environment in which contact occurs
C. Presence of extrapulmonary tuberculosis
D. Presence of laryngeal tuberculosis
E. Probability of contact with an infectious person
IV-114. Which of the following individuals with a known history of prior latent tuberculosis infection (without therapy) has the lowest likelihood of developing reactivation tuberculosis?
A. A 28-year-old woman with anorexia nervosa, a body mass index of 16 kg/m2, and a serum
albumin of 2.3 g/dL
B. A 36-year-old intravenous drug user who does not have HIV but is homeless
C. A 42-year-old man who is HIV-positive with a CD4 count of 350/μL on highly active
antiretroviral therapy
D. A 52-year-old man who works as a coal miner
E. An 83-year-old man who was infected while stationed in Korea in 1958
IV-115. A 42-year-old Nigerian man comes to the emergency department because of fevers, fatigue, weight loss, and cough for 3 weeks. He complains of fevers and a 4.5-kg weight loss. He describes his sputum as yellow in color. It has rarely been blood streaked. He emigrated to the United States 1 year ago and is an undocumented alien. He has never been treated for tuberculosis, has never had a purified protein derivative (PPD) skin test placed, and does not recall receiving BCG vaccination. He denies HIV risk factors. He is married and reports no ill contacts. He smokes 1 pack of cigarettes daily and drinks 1 pint of vodka on a daily basis. On physical examination, he appears chronically ill with temporal wasting. His body mass index is 21 kg/m2. Vital signs are blood pressure of 122/68 mmHg, heart rate of 89 beats/min, respiratory rate of 22 breaths/min, SaO2 of 95% on room air, and
temperature of 37.9°C. There are amphoric breath sounds posteriorly in the right upper lung field with a few scattered crackles in this area. No clubbing is present. The examination is otherwise unremarkable. His chest radiograph is shown in Figure IV-115 . A stain for acid-fast bacilli is negative. What is the most appropriate approach to the ongoing care of this patient?
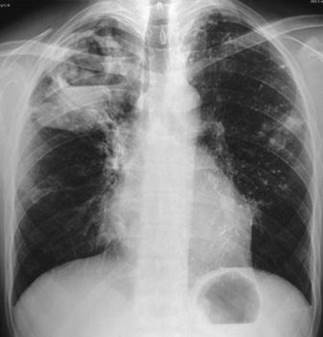
FIGURE IV-115
A. Admit the patient on airborne isolation until three expectorated sputums show no evidence of
acid-fast bacilli.
B. Admit the patient without isolation as he is unlikely to be infectious with a negative acid-fast
smear.
C. Perform a biopsy of the lesion and consult oncology.
D. Place a PPD test on his forearm and have him return for evaluation in 3 days.
E. Start a 6-week course of antibiotic treatment for anaerobic bacterial abscess.
IV-116. A 50-year-old man is admitted to the hospital for active pulmonary tuberculosis with a positive sputum acid-fast bacilli smear. He is HIV positive with a CD4 count of 85/μL and is not on highly active antiretroviral therapy. In addition to pulmonary disease, he is found to have disease in the L4 vertebral body. What is the most appropriate initial therapy?
A. Isoniazid, rifampin, ethambutol, and pyrazinamide
B. Isoniazid, rifampin, ethambutol, and pyrazinamide; initiate antiretroviral therapy
C. Isoniazid, rifampin, ethambutol, pyrazinamide, and streptomycin
D. Isoniazid, rifampin, and ethambutol
E. Withhold therapy until sensitivities are available.
IV-117. All of the following individuals receiving tuberculin skin purified protein derivative (PPD) reactions should be treated for latent tuberculosis EXCEPT:
A. A 23-year-old injection drug user who is HIV negative has a 12-mm PPD reaction.
B. A 38-year-old fourth grade teacher has a 7-mm PPD reaction and no known exposures to active
tuberculosis. She has never been tested with a PPD previously.
Date: 2016-04-22; view: 1930
| <== previous page | | | next page ==> |
| АМмЙАжDVT, Jeep venous [Ы)ЫкРЕ, pulmonary embolism. 2 page | | | АМмЙАжDVT, Jeep venous [Ы)ЫкРЕ, pulmonary embolism. 4 page |