
CATEGORIES:
BiologyChemistryConstructionCultureEcologyEconomyElectronicsFinanceGeographyHistoryInformaticsLawMathematicsMechanicsMedicineOtherPedagogyPhilosophyPhysicsPolicyPsychologySociologySportTourism
Keller distinguishes four types of edentulous jaws.
Ideal properties of impression materials
1. Non toxic and non irritant
2. Acceptability to the patient:
a) Setting time; b) Taste; c) Consistency.
3. Accuracy:
a) Surface reproducibility; b) Dimensional stability.
4. Use of material:
a) Ease of mixing ; b) Working time;
c) Setting time; d) Handling of the material.
5. Compatible with model materials
6. Economics of material
a) Cheap; b) Long shelf life;
c) Accuracy (save redoing impression)
Physical Phases of Alginate
§ The first phase is a sol (as in solution). In the sol phase, the material is in a liquid or semiliquid form.
§ The second phase is a gel. In the gel phase, the material is semisolid, similar to a gelatin dessert.
Alginates material
Properties
Good surface detail
Reaction is faster at higher temperatures
Elastic enough to be drawn over the undercuts, but tears over the deep undercuts
Not dimensionally stable on storing due to evaporation
Non toxic and non irritant
Setting time can depend on technique
Alginate powder is unstable on storage in presence of moisture or in warm temperatures
Causes for Distortion and Dimensional Change of Alginate
§ If an alginate impression is stored in water or in a very wet paper towel, the alginate will absorb additional water and expand. This condition is called imbibition.
§ If an alginate impression remains in the open air, moisture will evaporate from the material, causing it to shrink and distort. This condition is called syneresis.
§ Working time
• The time allowed for mixing the alginate, loading the tray, and positioning the tray in the patient's mouth.
§ Setting time
• The time required for the chemical action to be completed.
Instructions Taking a Complete Dental Impression
1. Select an appropriately sized dental tray for the upper teeth. The tray should fit snugly in the patient's mouth without causing strain on the jaws or teeth.
2. Mix the impression material according to the instructions on the package. Prepare a timer for the required set time as soon as you begin mixing. The set time includes the time it takes to mix the material and pour the tray, as well as the time in the patient's mouth. The impression begins to set as soon as it is mixed.
3. Apply adhesive to the inside of the dental tray. If the tray is perforated, the impression material will fill the holes and bind securely to the tray without adhesive.
4. Apply a small amount of wax to the outer edges of the dental tray. This will protect the patients mouth, as well as provide a tighter seal and a better impression.
5. Fill the dental tray with impression material.
6. Wipe a small amount of impression material on the occlusal surfaces of the upper teeth to prevent bubbling in the impression.
7. Use a dental mirror to gently pull the patient's cheek aside and insert the dental tray. The dental mirror is smaller than your fingers and allows you more maneuverability and the patient less discomfort.
8. Press the dental tray firmly onto the teeth, securing the tray tightly against the front and back teeth to get an accurate impression.
9. Allow the impression material to set. Remember to remain relaxed. Call out the time remaining to let your patient know exactly where he or she is in the process.
10. Remove the tray from the patient's mouth when the timer you set in Step 2 goes off. Wiggle the tray slightly to loosen the dental tray from the teeth, but do not wrench as this will cause defects in the mold.
11. Inspect the mold to determine that there are no bubbles and that all occlusal surfaces have been accurately represented.
12. Disinfect the mold using an antibacterial spray and rinse.
13. Wrap the mold in a wet paper towel and place in a plastic bag with the patient's name on it.
TEST FOR INITIAL LEVEL OF KNOWLEDGE
1. For a patient 28 years produced laminar RPD. Objectively: the teeth are high, stable. Alveolar process moderately atrophied. Which impression material to use in this case?
A. Upin *
B. Repin;
C. Dentol-C;
D. Gypsum;
E. Sielast-69.
2. A patient 49 years with generalized periodontitis moderate severity. Dentist made non-removable dentures. Which impression material should be applied in this case?
A. Upin, stomalgin *
B. Gypsum dentol-C;
C. Stens, ortokor;
D. Sielast-69 stomafleks;
E. Akriloksid, Protakril-M.
3. Describe the main advantages of alginate materials:
A high precision, low shrinkage;
B. Easy to use in the clinic;
C. The high ductility and low elasticity;
D. Strong connection with perforated impression trays, low toxicity;
E. High flexibility. *
4. A patient 75 years with edentulous jaws, used to dentures 10 years. Objectively: the lower third of the face is reduced, alveolar process on the upper and lower jaws are atrophied, the palate is flat, mucous membrane atrophied. What kind of impression material is best to use for functional impressions in this case?
A. Alginate material
B. Stens;
C. Gypsum;
D. Ortokor;
E. The silicone material.*
5. Which difference between functional and anatomic impression:
A. Anatomical print complements functional;
B. The differences between them;
C. The difference between them is negligible
D. They have difference techniques of taking;*
E. Functional anatomy print supplements.
6. One of the stages of complete dentures is adjustments of individual tray and removal of functional impression. Which of these materials is carried for edges of individual tray?
A. Gypsum;
B. Ortokor;*
C. Hromopan;
D. Tiodent;
E. Stomalgin.
7. The patient 60 years old in order to prosthetics. Objective: partially edentulous jaws. Other teeth I-II degree of mobility. Dentist will make partial denture on the lower jaw. Which impression material prefer?
A. Stomalgin *
B. Ortokor;
C. Sielast;
D. Stens;
E. Gypsum.
8. Impression its:
A printout of the upper and lower jaw and teeth
B. Displaying oral tissues for impression materials;
C. Positive display tissue prosthetic area
D. Negative display tissue prosthetic area;*
E. An impression of the teeth, the mucous membranes, mouth on impression materials.
9. M.A. Napadov divides impression materials into the following groups:
A plaster, silicone, alginate, polymerized, thermoplastic;
B. crystallized, polymerized, elastic, silicone, thermoplastic;
C. curatives, firm, elastic, thermoplastic, hydrocolloid;
D. Hard, soft, flexible, thermoplastic, hydrophobic
E. hardening, thermoplastic, elastic*
Special-purpose Training Tests for study the topic level testing
1. The patient is made sintered metal bridge on 47, 45 teeth. Preparation of teeth done ledge. Which of the materials will get a quality impression?
A. Repin;
B. Stomalgin;
C. Sielast-05 *
D. Dentafol;
E. Ortokor.
2. Specify the main drawback of alginate materials:
A. swelling in the water
B. Low elasticity;
C. Significant and rapid shrinkage;*
D. Low accuracy;
E. greater strength
3. Which of the following dental materials is an example of an aqueous elastometric?
A. Impression compound
B. ZOE impression paste
C. Polysulfide
D. Irreversible hydrocolloid *
E. Addition silicone
4. Which of the following is an example of an inelastic impression material?
A. Polysulfide
B. ZOE impression paste *
C. Alginate
D. Addition silicone
5. A 73-year-old patient consults a dentist about total edentia. Objectively: there is insignificant regular atrophy of the alveolar process of mandible, the process is covered with mucous membrane of moderate elasticity. According to Keller's classification, such manifestations are characteristic for the following type of edentulous jaw:
A Second
B Third
C Fifth
D First *
E Fourth
6. Women 32 year-old went to the doctor in order to prosthetics. After a physical examination selected prosthesis with metal-ceramic crowns. Which impression material should be used:
A. "Repin"
B. "Stomafleks" *
C. "Stomalgin"
D. "Stens"
E. "Ortokor"
7. Woman has not been to the dentist for several years. It was found that she needed extensive restorative treatment to which she agreed. You were asked to take impressions as the first step of her care. The impression material of choice would be:
A. agar
B. alginate *
C. dental impression compound
D. addition silicone
Keller distinguishes four types of edentulous jaws.
At the first type of the alveolar process and uniformly slightly atrophied. At this early rounded alveolar ridge is a good basis for the prosthesis and it restricts the freedom of movement in the direction of the displacement. The points of attachment of muscles and folds of mucous membrane located at the base of the alveolar bone. This type of jaw observed in that case, if the teeth are removed at the same time and atrophy of the alveolar process is slow. It is most convenient for the prosthesis, although relatively rare.
The second type is characterized by a significant expression, but uniform atrophy of the alveolar bone. Alveolar ridge barely rises above the bottom of the oral cavity, representing in the anterior narrow, sometimes sharp as a knife, education is of little use under the base for the prosthesis. The insertions of the muscles are almost at the level of the ridge. This type of lower edentulous jaw is very difficult to obtain a stable prosthesis and functional result, since there are no conditions for anatomical retention, and the high position of the points of attachment of muscles in their reduction leads to a shift in the prosthesis to his bed. Use of a prosthesis with the often painful because of the sharp edge of the internal oblique line and in some cases, success is achieved only prosthetics after smoothing.
The third type is characterized by severe alveolar atrophy of alveolar bone in the lateral parts with relative preservation of alveolar bone in the anterior part. This type of alveolar bone occurs with early removal of posterior teeth. It is favourable for the prosthesis, because in between the sides of the external and internal oblique lines are flat, almost concave surfaces are free from points of attachment of muscles, and the presence of alveolar bone in the anterior region of the displacement of the prosthesis prevents him in the anterioposterior direction.
In the fourth type of atrophy of the alveolar process is most marked in front with relative preservation of it in the sides of the lower jaw. As a result, the prosthesis loses support in the anterior and slides forward. Assessment of the mucous membrane of edentulous jaws. Changes that develop in the mouth after tooth extraction capture not only the alveolar process, and the mucous membrane covering them, and the hard palate. They can be expressed in the form of atrophy, wrinkling, change the position of the fold transition to the alveolar ridge. The nature and extent of these changes are related not only to the loss of teeth, but also the causes which led to their removal. General and local diseases, age-related changes also affect the nature and extent of the restructuring of the mucous membrane after tooth extraction. Knowledge of the characteristics of tissue covering the prosthetic area, is of great importance both to select the method of prosthetics, and to prevent harmful effects of the prosthesis on the supporting tissue.
Supple focus draws on the state of mucous membrane and releases 4 classes. At the first class, both on the upper and lower jaw have a pronounced alveolar ridge, covered slightly pliable mucosa. The sky is also covered with an even layer of the mucous membrane, uniformly supple in the posterior third. Natural folds of mucous membrane (lip, cheek and bridle cheek bands) as the upper and lower jaw are far enough from the top of the alveolar bone. This class is a convenient mucosal support for the prosthesis, including a metal base. The second class is characterized by atrophied mucous membrane covering the alveolar process and the sky as thin as a strained layer. The insertions of natural folds are located closer to the top of the alveolar process than first class. Dense and thinned mucosa is less convenient to support the denture, especially with a metal base. In the third class of the alveolar process and the posterior third of the hard palate is covered loosened mucosa. Such a condition often found lining the low alveolar ridge. Patients with this mucous sometimes require preliminary treatment. After prosthesis should adhere strictly to the use of prosthesis and always under medical supervision. Fourth grade is characterized by moving tissues of the mucous membrane, located longitudinally and easily slips when slightly off impression material. Strands be constrained by making it difficult or impossible to completely use a prosthesis. These folds are observed mainly in the lower jaw, mainly in the absence of alveolar bone. The same type of alveolar bone is to "hang out" soft ridge. Sometimes the prosthesis can be made only after the removal of the ridge. Mucosal pliability, as seen from the classification Supple, is of great practical importance.
Based on the varying degrees of flexibility of the mucous membrane, Lund allocates hard palate 4 areas:
1. area of the sagittal suture;
2. alveolar bone;
3. portion of the hard palate in the transverse folds;
4. posterior third of the hard palate.
The mucosa of the first zone is thin, has no submucosa. Suppleness of her minuscule. This site is named Lund medial (middle) of the fibrous zone. The second zone captures the alveolar bone and is also covered by mucous membrane, and almost devoid of the submucosal layer. Is peripheral fibrous zone. The third zone is covered with mucous membrane, which has a high degree of compliance. The fourth area - the back third of the hard palate, a submucosal layer rich in mucous glands and contains little fat. This layer is soft, springy in the vertical direction has the highest degree of compliance and called glandular area. Most researchers explain yielding mucosa of the hard palate and alveolar structural features of the submucosal layer, in particular, located in its fiber and oil glands. Different point of view, we adhere to, linking vertical compliance of mucosal surfaces with a thick jaw bones submucosal vasculature. It was filled with their ability to rapidly emptied and as quickly fill with blood can create conditions for reducing the volume of tissue. Lots mucosa of the hard palate with extensive vascular fields, has therefore, as it were spring properties, called buffer zones. The histological and topographical studies (V.S. Zolotkov) found that the mucous membrane covering the alveolar process and part of the hard palate to the sagittal suture, has small vascular fields and buffer properties because almost none. In areas of the mucous membrane located between the base of the alveolar process and the middle zone are dense vascular field, which increases the density of blood vessels in the direction of the line "A". So that the buffering capacity of the mucous membranes of the hard palate in the direction of the line "A" is also increasing. Pliability mucosa of the hard palate studied in detail V.I. Kulazhenko by electron-vacuum apparatus. He found that it is in the range of 0.5 to 2 mm. These V.I. Kulazhenko point of compliance mucosa of the hard palate with the topography of the same buffer zones on E.I.Gavrilov.
Buffering capacity of the mucosa of the upper jaw prosthetic field in life change dramatically, due to changes in blood vessels under the influence of age, metabolic, infectious and other diseases. The state of the vessels of envy not only yielding mucosal surfaces of the hard palate, but the nature of its response to the effects of the prosthesis. In the origin of changes in the mucosa, atrophy of the alveolar process, is often observed in long-term use of prosthetic vessels play a major role.
Date: 2015-01-02; view: 7053
| <== previous page | | | next page ==> |
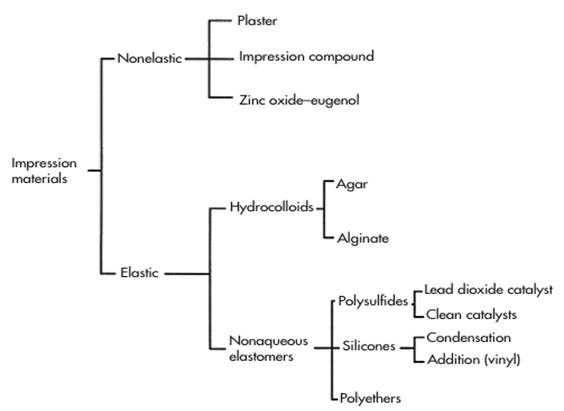
| Classification of impression materials | | | Topic 84.1. Benchmarking to build the bite. |